· 5 min read
Virologists consider response to Zika
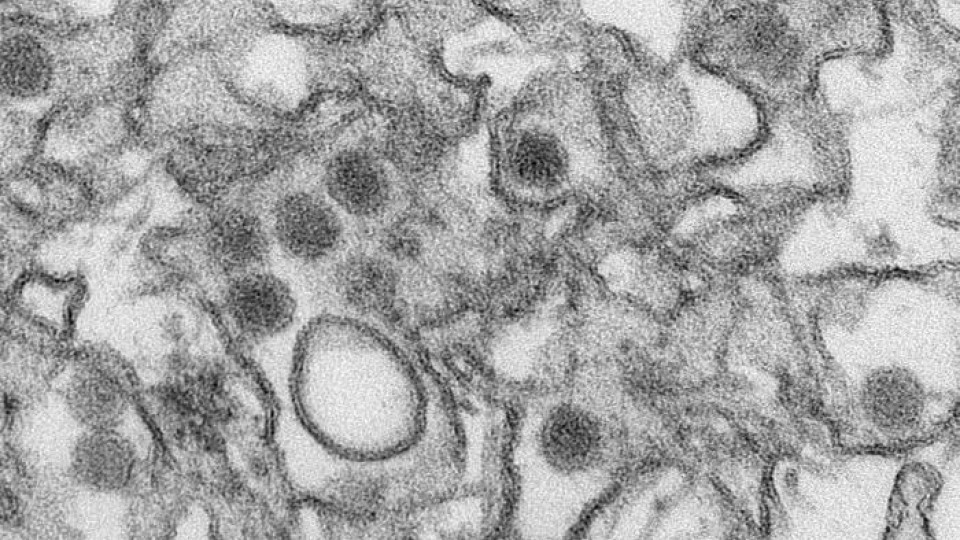
Nebraska researchers are watching closely in preparation to join the fight against the spread of Zika virus in Latin America and the Caribbean.
Asit K. Pattnaik, a University of Nebraska-Lincoln professor at the Nebraska Center for Virology, said he has been conferring with colleagues to begin researching the little-studied virus in hopes of eventually developing a vaccine or an anti-viral medication.
“Although the virus has been around for many years in Africa and Asia, it has spread to Brazil and other Latin American countries only recently,” Pattnaik said. “Not many laboratories within the (United States) actually are working on this virus at this time.”
The World Health Organization has warned that Zika is likely to spread to all countries in the Americas except for Canada and Chile. That’s because Aedes mosquitoes, the main vector for Zika virus transmission, live in all but those two countries.
A burst of cases that began in Brazil last May has spread to more than 20 nations and is tied to nearly 4,000 cases of microcephaly in babies born to women who contracted the virus early in pregnancy. Microcephaly is a birth defect that results in abnormally small craniums and underdeveloped brains.
About 20 cases have been reported in the United States, but health officials say all so far appear to involve returning travelers. It does not yet appear that the virus has been transmitted in the United States. The cases include a woman who had traveled to Brazil and later gave birth in Hawaii to a baby with microcephaly. U.S. health officials have said a major outbreak is unlikely in the country because the Aedes mosquito favors tropical areas and because widespread use of air conditioning enables people to more easily avoid contact with the mosquito.
According to the Centers for Disease Control and Prevention, the virus was first detected in a monkey in the Zika forest in Uganda, in 1947. Human cases were reported sporadically in African and Asian countries before the first documented outbreak in Micronesia in 2007.
10 things to know about Zika right now
Pattnaik, who studies viral pathogens, said the first step for scientists in the Nebraska Center for Virology would be to replicate the virus so that it can be manipulated to develop a vaccine. It would be similar to previous work done with the Porcine Respiratory and Reproductive Syndrome virus. Researchers have applied for a patent for a vaccine against that virus.
“Our goal is to develop vaccines and we’ve made major headway on that in collaboration with faculty at the center,” Pattnaik said.
Established in 2000, the virology center combines the expertise of the state’s leading biomedical research institutions – UNL, the University of Nebraska Medical Center and Creighton University. Its research focused on human, plant and animal viruses.
Much needs to be learned about how the virus arrived in Brazil and how it has spread from there, Pattnaik said. Some believe that Zika could have been carried to Brazil by World Cup fans two years ago.
The link between Zika and the occurrence of microcephaly is circumstantial, Pattnaik said. Researchers have yet to understand the mechanism that triggered the birth defect.
A harbinger of climate-related outbreaks?
Daniel Brooks, a parasitologist and senior research fellow with UNL’s H.W. Manter Laboratory of Parasitology, said he is concerned the Zika outbreak is a sign of things to come as climate change alters the relationships between pathogens and their hosts.
In a 2015 article, Brooks warned that humans can expect more infectious disease to emerge as climate change shifts habitats and brings wildlife, crops, livestock and humans into contact with new pathogens.
“This is exactly what we’ve been ranting about for 25 years,” Brooks said. “These things are popping up and moving faster than the bureaucracies can track them, much less do anything effective.”
Brooks said authorities should not dismiss the possibility of a significant Zika outbreak in the United States. Changes in temperature and rainfall patterns create new habitats for disease carriers like mosquitoes.
“It’s inevitable that the southern mosquitoes will move north (as temperatures in northern areas grow warmer,)” he said.
Zika virus turning up in new places also hints that other pathogens, like those that cause malaria, yellow fever and Dengue fever, could crop up more frequently.
“We’ve got to do something about the Zika virus now,” Brooks said. “But we should have anticipated this long ago.”
Along with research for vaccines and anti-viral drugs, public health officials should investigate whether the Zika virus has “jumped” from Aedes mosquitoes to other North American mosquito species and whether there are non-human animals that might serve as “reservoirs” for the virus, he said. Such knowledge is key to implementing mosquito control programs and other mitigation policies that could buy time until vaccines are developed.
Several countries have recommended that women avoid getting pregnant until after the outbreak abates. But it is easier to attack mosquito populations than it is to get humans to refrain from having children, Brooks said.
“We need to consider every element of the pathway of transmission for things like Zika to help identify weak links in the chain,” he said. “Our goal is to anticipate and mitigate the effects of emerging diseases that will become ever more problematical and expensive as the effects of climate change continue to manifest themselves.”










